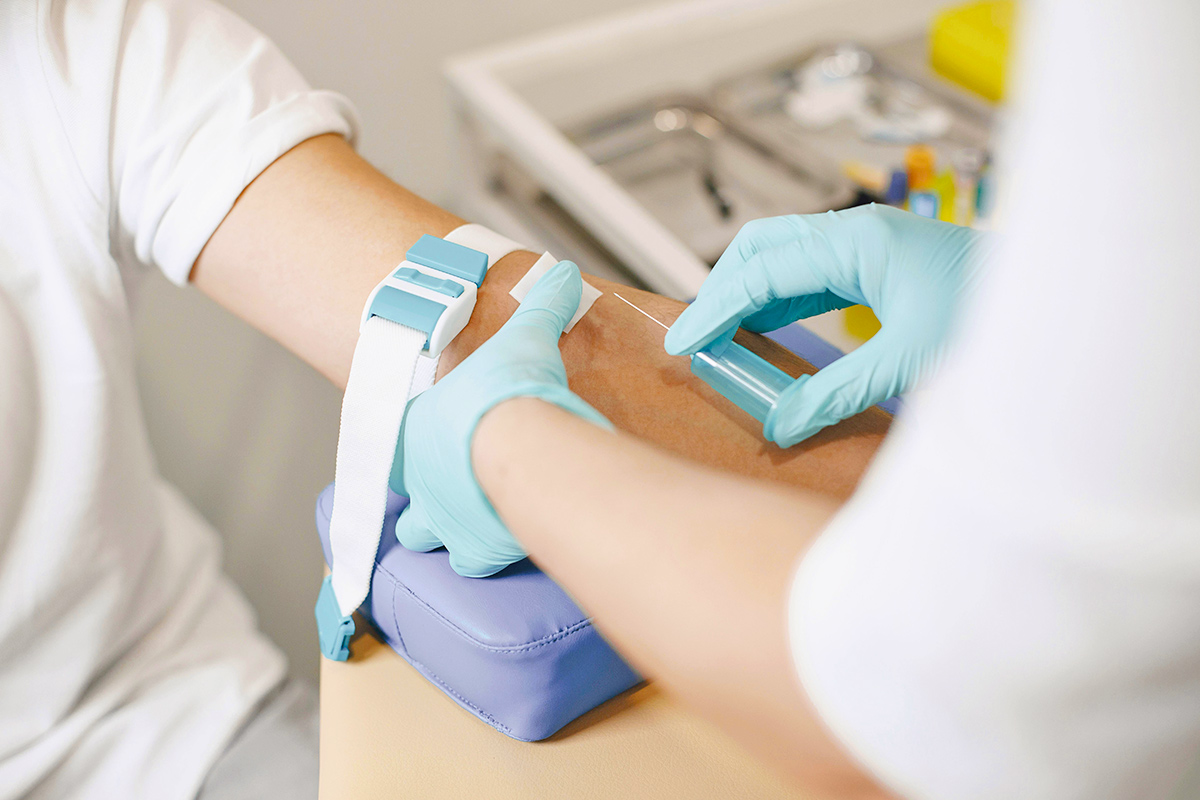
Most of us assume that if we get routine bloodwork and “everything looks normal,” we’re in the clear. But many doctors say this reassurance is misleading. Standard lab panels often miss key markers that may reveal problems earlier, sometimes years before symptoms appear, allowing you to take better control of your health. From hidden heart risks to silent vitamin deficiencies, there are important tests your doctor may not be ordering, but perhaps should. We spoke with several medical professionals to help us identify which overlooked screenings could provide a more complete picture of your health.
Fasting Insulin
Dr. Olga Bachilo, M.D., FACS, a board-certified plastic surgeon and owner of Glamour Plastic Surgery and Med Spa in Houston, Texas, says fasting insulin is the most commonly missed test in a panel. Most doctors order a fasting glucose test instead, which measures the amount of sugar (glucose) in your blood after fasting for eight to 12 hours. It’s a go-to method for screening for diabetes.
However, according to Dr. Bachilo, glucose levels may creep up but remain in the normal range for years while insulin levels rise to compensate. Insulin is a hormone produced by the pancreas that helps move blood glucose from your bloodstream into your cells, where it can be used for energy. The pancreas creates more insulin in response to increased glucose to keep blood sugar levels in the “normal” range, and it’s at this point that a fasting insulin test could detect what’s called “insulin resistance,” which is one step before prediabetes. Dr. Bachilo notes that she often sees surgery patients whose primary care doctors didn’t notice an increase in their insulin levels, despite common symptoms such as midsection weight gain and lethargy.
In some cases, insulin resistance can go on undetected for years, but over time, the pancreas cannot keep up and blood sugar levels rise. At this point, it’s called “prediabetes,” as blood sugar levels are elevated but not yet high enough for a Type 2 diabetes diagnosis. Fortunately, it’s possible to reverse both insulin resistance and prediabetes through nutrition, physical activity, weight loss, and sleep and stress management.
But “by the time glucose is elevated,” Dr. Bachilo says, “the metabolic damage is already done.” A high blood glucose test result, called hyperglycemia, usually results in a diabetes diagnosis. This is much harder to reverse than insulin resistance and prediabetes, and is typically managed through injected insulin or oral diabetes medication, along with lifestyle changes.
A fasting insulin test will identify the problem earlier, to the point where lifestyle changes may resolve it. Your doctor can help you set up the test, which is similar to a fasting glucose test, where you don’t eat for a specified period, then have a blood test.

Vitamin D
Dr. Suzanne Borkowski, M.D., board-certified psychiatrist in private practice at Resonance Psychiatry, emphasizes the importance of vitamin D. “While several tests are routine during a psychiatric intake, I have found that a vitamin D level test offers the highest yield, regardless of a patient’s demographic or medical history,” she says. “In my experience ordering this test hundreds of times in the past five years alone, fewer than 10 patients have returned results within the normal range.”
Reader Favorites
According to the Cleveland Clinic, approximately 35% of U.S. adults have vitamin D deficiency, as do 1 billion people worldwide. This is because many people don’t get enough of the vitamin through diet and sun exposure, and for the most part, patients don’t realize they’re deficient.
The long-term impacts of low vitamin D are serious. It’s a known risk factor for depression, epilepsy, and neurocognitive decline, including Alzheimer’s disease, according to Dr. Borkowski. “It has also been associated with various cancers, cardiovascular diseases, Type 2 diabetes, and immune system dysregulation,” she says, making it an important metric to watch to decrease your risk of long-term health issues. “The importance of maintaining normal vitamin D levels for lifelong health cannot be overstated.”
Signs and symptoms of a deficiency include fatigue, bone pain, muscle weakness, aches or cramps, and mood changes.
Your health care provider can order a blood test separate from routine lab work to check your levels. According to Dr. Borkowski, people diagnosed with a deficiency often don’t get rechecked to make sure their levels have rebounded, so if you’re deficient, make sure you don’t skip that step.
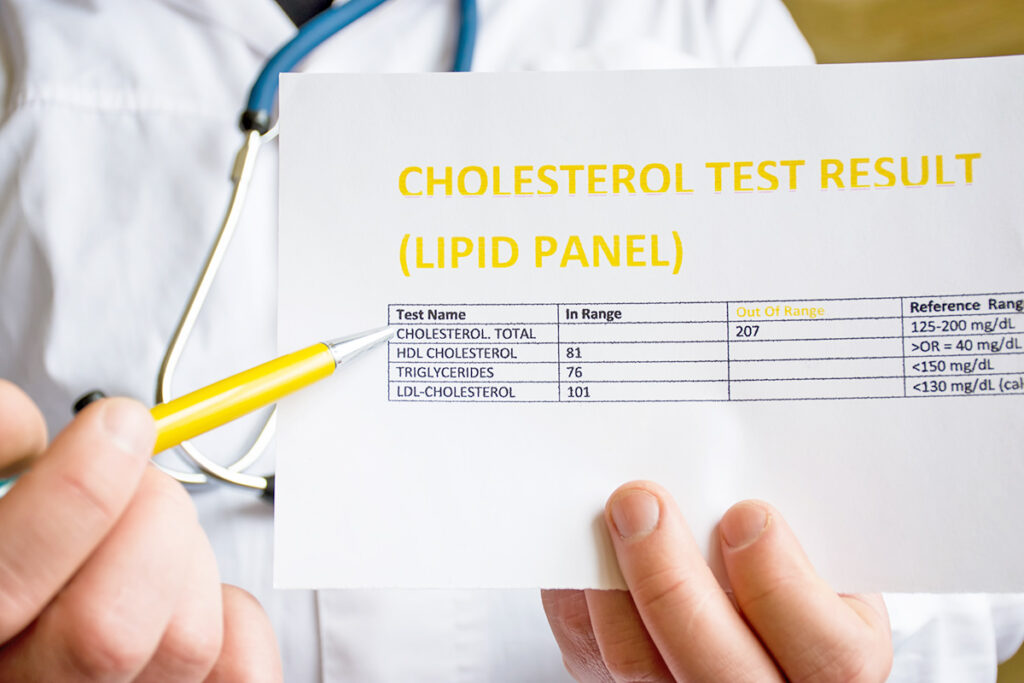
Lipoprotein(a)
According to Dr. Nneoma Oparaji, M.D., DipABLM, DABOM, a triple board-certified physician in obesity, lifestyle, and internal medicine, the one test that doctors aren’t ordering enough is Lipoprotein(a). According to Dr. Oparaji, “Lp(a) is a genetically inherited cholesterol particle that independently increases the risk of heart attack and stroke.” Despite this fact, testing for Lp(a) is not included in routine cholesterol panels. Dr. Oparaji calls it the “missing puzzle [piece] in high-risk patients who otherwise have a ‘normal’ cholesterol test.”
Dr. Oparaji says that one in five people globally have elevated Lp(a) levels, making it one of the biggest gaps in preventative care today. She recommends that everyone get an Lp(a) test at least once as an adult. “This test is important because it demonstrates the risk that we inherit and not the risk we earn,” she says. “It is a single test that gives you an early insight into your lifelong risk of heart disease.”
Testing early, before symptoms arise, helps shift treatment from “reactive care to proactive prevention.” Dr. Oparaji also notes that postmenopausal women with elevated Lp(a) levels may be at a higher risk of heart disease. To test your Lp(a) levels, make a request to your doctor. It’s a simple, yet nonstandard, blood test.

Sleep Apnea
Dr. Max Kerr, DDS, D-ABDSM, a dentist who specializes in the treatment of sleep apnea and the owner of Sleep Better Austin, wishes more doctors would order home sleep tests (HSTs). “Sleep-disordered breathing (SDB), primarily obstructive sleep apnea (OSA), is highly prevalent, affecting 20% to 30% of adults, with rates up to 90% in certain elderly populations,” he says.
Untreated sleep apnea can impact your daily life, from daytime fatigue to memory and cognitive issues. It may also have devastating long-term effects on your health, including high blood pressure and a higher risk of heart disease, stroke, Type 2 diabetes, and depression. “Sleep apnea is extremely underdiagnosed, [yet it] affects so much of our health,” he says. “Home sleep testing should be as ubiquitous as regular blood panels.”
HSTs can be performed at home by placing small sensors on the body to track breathing patterns, oxygen levels, and heart rate while you sleep. Then a sleep specialist reviews the data, providing you with better insight into your sleep quality.
Methylmalonic Acid and Homocysteine
As Dr. Cooper Stone, D.O., a clinical assistant professor of psychiatry and behavioral health at the University of Pennsylvania, explains, there isn’t just one under-tested lab; there are many. However, he lists several that he checks as a psychiatrist, including vitamin D, an iron panel with ferritin (to monitor anemia), and methylmalonic acid and homocysteine levels.
A methylmalonic acid test is used to diagnose a vitamin B12 deficiency, while a homocysteine test measures levels of vitamin B6, vitamin B12, and folate. Checking both is important because “a B12 deficiency and a folate deficiency will present with a high homocysteine level,” Dr. Stone says. “To differentiate the two, only a methylmalonic acid level will be elevated in a B12 deficiency.”
Vitamin B12 helps make red blood cells and DNA, and it’s derived from what you eat — your body can’t make the nutrient on its own. Symptoms of a deficiency may include tiredness, gastrointestinal issues, lack of appetite, weight loss, mouth sores, and pale skin. It’s also associated with serious neurologic symptoms, including memory issues, numbness and tingling, and proprioception problems.
“For me, the most important thing to remember is that you can have a normal vitamin B12 and a folate level and still be deficient,” Dr. Stone says. This is because normal ranges are based on population averages, not individual needs. If a patient is at the lower end of the B12 or folate range, it may not be flagged as abnormal, and a clinician may miss it. This is why it’s important to be proactive about your health and ask your doctor follow-up questions if any of your levels, such as B12, are on the low end of the “normal” range. Supplementation may still be right for you.
Treating these deficiencies with supplementation can reduce symptoms and long-term impacts. Talk to your doctor about blood tests for methylmalonic acid and homocysteine if you have concerns about your vitamin B12 and/or folate levels.
Featured Image Credit: © Gustavo Fring/Pexels.com
More From Our Network
Better Report is part of Inbox Studio, an email-first media company. *Indicates a third-party property.